Medicare Enrollment Deadlines
When Can You Enroll? Understanding Your Medicare Enrollment Deadlines
When it comes to Medicare, when you enroll is just as important as what you enroll in. Signing up at the right time helps you avoid lifelong penalties and ensures you don’t have gaps in your health coverage. We’ve broken down the key periods you need to know about.
YOUR 7-MONTH WINDOW
Your First Medicare Enrollment Deadline:
The Initial Enrollment Period (IEP)
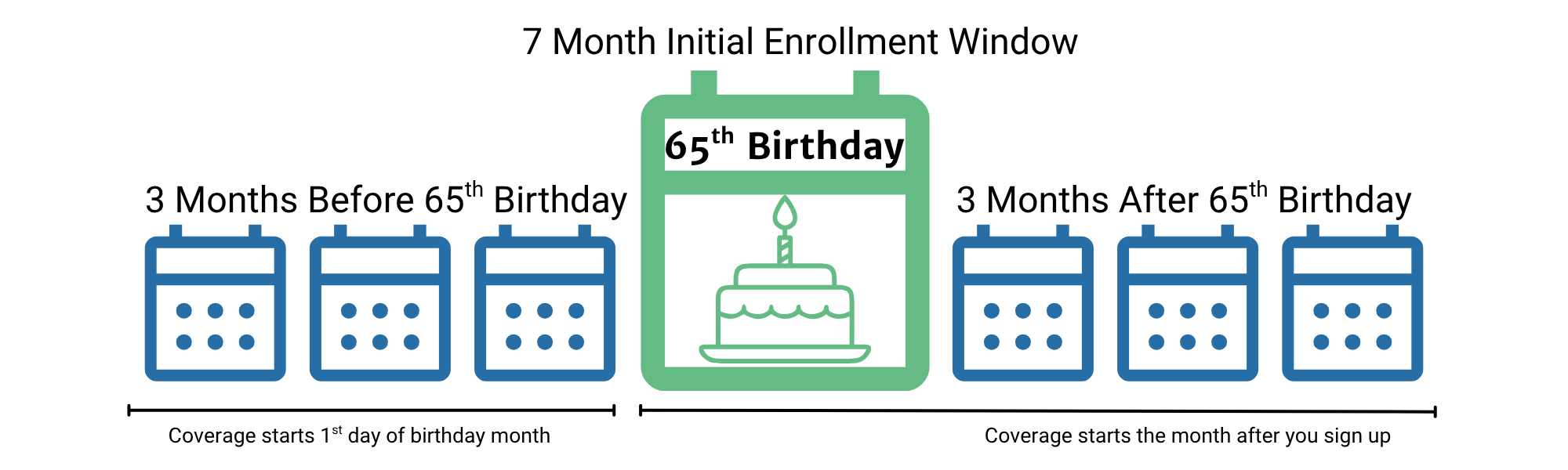
For most people, your Initial Enrollment Period is your main window to sign up for Medicare when you turn 65. It’s a 7-month period that is unique to you, centered around your birthday month.
When your coverage begins depends on when you sign up within this window. To ensure your coverage starts right when you turn 65, it’s best to enroll during the first 3 months of your IEP. (Note: If your birthday is on the 1st of the month, your coverage will start a month earlier!)
However, if you enroll during your birthday month or in the last 3 months of your IEP, your coverage will start on the first day of the month after you sign up. Understanding this timeline is key to avoiding any unexpected gaps in your health coverage.
If you’re under 65 and become eligible for Medicare due to a disability, your 7-month IEP is typically centered around your 25th month of receiving disability benefits.
YOUR ANNUAL CHECK-UP
The Annual Enrollment Period (AEP):
Your Yearly Time to Review & Change
Once you’re enrolled in Medicare, you get a yearly opportunity to review your coverage and make changes. This is known as the Annual Enrollment Period (AEP), and it happens at the same time every year.
This is the perfect time to sit down with us for your yearly Medicare review to make sure your current plan is still the best fit for your health and budget for the year ahead.
When is it?
AEP runs from October 15 to December 7 each year.
What can you do?
During this time, you can join, switch, or drop a Medicare Advantage Plan or a Medicare Part D Prescription Drug Plan.
Can you change your mind?
Yes, you can make as many changes as you need to during AEP. Just remember, the last choice you make before the December 7th deadline is the one that will become your plan for the new year.
When does new coverage start?
Any changes you make during the AEP will take effect on January 1 of the following year.
FOR LIFE’S UNEXPECTED CHANGES
Special Enrollment Periods (SEPs):
When You Can Change Plans Mid-Year
Sometimes, life happens outside of the regular enrollment seasons. In certain situations, you may qualify for a Special Enrollment Period (SEP), which gives you an opportunity to join, switch, or drop your Medicare Advantage or Part D plan outside of the Annual Enrollment Period. These are triggered by specific qualifying life events.
You move into or out of an institution like a skilled nursing facility or long-term care hospital.
You’re diagnosed with a severe or chronic condition and a Medicare Chronic Care Special Needs Plan (SNP) is available for you.
You move to a new address that isn’t in your current plan’s service area.
You lose other creditable prescription drug coverage, such as from an employer or union.
You qualify for Extra Help to pay for your Part D costs.
SEP rules and timing can be specific, so if you’ve recently had a major life change, it’s a good idea to talk to an expert. We can help you understand if you qualify for a Special Enrollment Period and guide you through your options.
Other Important Enrollment Deadlines to Know
Sometimes, life happens outside of the regular enrollment seasons. In certain situations, you may qualify for a Special Enrollment Period (SEP), which gives you an opportunity to join, switch, or drop your Medicare Advantage or Part D plan outside of the Annual Enrollment Period. These are triggered by specific qualifying life events.
General Enrollment Period
(GEP)
If you missed your Initial Enrollment Period (IEP) and don’t qualify for a Special Enrollment Period, the GEP is for you. It runs from January 1 to March 31 each year.
During this time, you can sign up for Part A and/or Part B. Your coverage will begin the first day of the month after you sign up. Keep in mind, a late enrollment penalty may apply.
Medicare Advantage Open Enrollment Period (MA-OEP)
This period is only for people who are already enrolled in a Medicare Advantage plan. From January 1 to March 31 each year, you get a one-time chance to:
Why Enrolling on Time is So Important
Understanding Late Enrollment Penalties
We emphasize the enrollment periods because if you miss your window to sign up and don’t have other creditable coverage, you could face late enrollment penalties.
These penalties are typically added to your monthly premium payments for Part A (if you have to buy it), Part B, and Part D. For Part B and Part D, these penalties are usually for as long as you have the coverage, so they can last a lifetime. Navigating your timeline correctly is the best way to avoid these extra costs.
Ready to Enroll? Let Us Help!
Navigating Medicare Enrollment can be complex. Our experienced team is here to guide you through the process, ensuring you enroll at the right time and in the right plan for your needs.

